The intricate relationship between diabetes mellitus and glaucoma presents a significant challenge in ophthalmology. A growing body of research explores the mechanisms and clinical implications of this association, consistently indicating that individuals with diabetes face an elevated risk of developing various forms of glaucoma, particularly open-angle glaucoma.
Understanding the Diabetic-Glaucoma Connection
Diabetes, a chronic metabolic disorder characterized by hyperglycemia, profoundly affects multiple organ systems, including the delicate structures of the eye. While diabetic retinopathy is a well-recognized complication, the impact of diabetes extends beyond the retina, influencing intraocular pressure (IOP) regulation and optic nerve health—both critical factors in glaucoma pathogenesis.
ℹ️ Elevated Risk
Epidemiological studies have repeatedly shown a higher prevalence of glaucoma in diabetic populations, often two to three times greater than in non-diabetic individuals. This heightened vulnerability is attributed to several pathophysiological pathways.
Pathophysiological Mechanisms
Chronic hyperglycemia contributes to oxidative stress, inflammation, and microvascular dysfunction, all of which can lead to the degeneration of retinal ganglion cells and optic nerve damage characteristic of glaucoma.
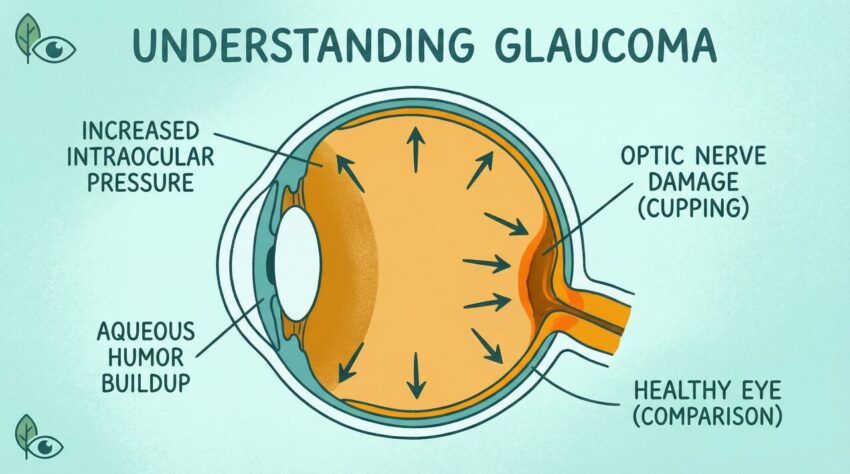
One primary mechanism linking diabetes to glaucoma involves alterations in aqueous humor dynamics. Diabetes can impair the function of the trabecular meshwork, the main outflow pathway for aqueous humor, leading to increased resistance and elevated IOP. Furthermore, advanced glycation end products (AGEs) and other diabetic byproducts can alter the extracellular matrix within the trabecular meshwork, further impeding aqueous outflow.
Diabetic neuropathy can also compromise the autonomic nervous system’s control over ocular blood flow, potentially reducing perfusion to the optic nerve head. Diminished blood supply to the optic nerve, a common feature in glaucoma, can exacerbate neuronal damage and accelerate vision loss in diabetic patients.
Diabetic Retinopathy and Neovascular Glaucoma
The connection between diabetic retinopathy and glaucoma is particularly crucial. Proliferative diabetic retinopathy (PDR), the most advanced stage of diabetic retinopathy, can directly cause neovascular glaucoma. In PDR, abnormal new blood vessels proliferate on the iris and in the angle of the eye, obstructing aqueous humor outflow and leading to a severe, often painful, increase in IOP. This form of glaucoma is notably aggressive and challenging to manage.
✅ Therapeutic Insights
Recent research highlights the potential protective effects of certain diabetes medications against glaucoma. Studies suggest that GLP-1 receptor agonists (GLP-1RAs) may lower glaucoma risk, and metformin has been associated with a protective effect on open-angle glaucoma.
Clinical Management and Future Directions
Clinical guidelines underscore the importance of regular, comprehensive eye examinations for individuals with diabetes, including dilated fundus examinations and IOP measurements. Early detection and timely intervention are paramount for preserving vision in diabetic patients at risk of or diagnosed with glaucoma. Management typically involves a multidisciplinary approach, integrating optimal glycemic control, blood pressure management, and lipid control with glaucoma-specific treatments such as topical medications, laser therapy, or surgery.
Despite accumulating evidence, some epidemiological studies have presented inconsistencies in the diabetes-glaucoma association, leading to ongoing scientific debate and further research. These discrepancies may arise from variations in study design, diagnostic criteria for both conditions, and the diverse populations studied. Nevertheless, the prevailing consensus identifies diabetes as a significant risk factor for glaucoma, necessitating vigilant screening and management.
✅ Key Takeaway
Diabetes mellitus substantially elevates the risk of glaucoma through a complex interplay of metabolic, vascular, and neurological factors. Proactive screening, early diagnosis, and comprehensive management remain essential in mitigating the devastating impact of glaucoma in the diabetic population.