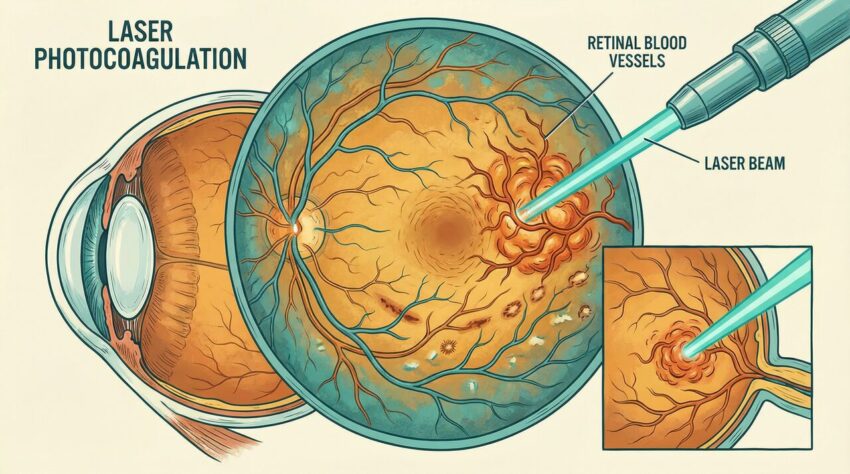
Diabetic retinopathy (DR) stands as a leading cause of vision impairment and blindness among working-aged adults globally. Characterized by damage to the blood vessels of the light-sensitive tissue at the back of the eye, the retina, DR progresses through stages, from mild non-proliferative diabetic retinopathy (NPDR) to severe proliferative diabetic retinopathy (PDR). The advent of laser photocoagulation revolutionized the management of DR, offering a critical intervention to preserve vision and prevent irreversible sight loss. This article delves into the mechanisms, types, indications, and efficacy of laser treatment for retinopathy, emphasizing its pivotal role in contemporary ophthalmological practice.
Understanding Diabetic Retinopathy and the Rationale for Laser Intervention
Diabetic retinopathy arises from prolonged hyperglycemia, which leads to microvascular damage within the retina. This damage manifests as microaneurysms, hemorrhages, hard exudates, and cotton wool spots in NPDR. As the disease progresses to PDR, new, fragile blood vessels (neovascularization) proliferate on the surface of the retina or optic disc. These abnormal vessels are prone to bleeding, leading to vitreous hemorrhage, and can also cause tractional retinal detachment, both of which severely impair vision. [1]
The primary rationale for laser intervention in DR is to halt or slow the progression of the disease by targeting these pathological changes. Laser photocoagulation works by creating controlled burns on the retina, which in turn reduces the metabolic demand of the peripheral retina, thereby decreasing the production of vascular endothelial growth factor (VEGF) and other pro-angiogenic factors. This reduction helps to regress neovascularization and prevent further leakage from abnormal vessels. [2]
Types of Laser Photocoagulation
Two main types of laser photocoagulation are employed in the treatment of diabetic retinopathy:
1. Panretinal Photocoagulation (PRP) / Scatter Laser Surgery
Panretinal photocoagulation, often referred to as scatter laser surgery, is primarily indicated for proliferative diabetic retinopathy (PDR) and severe non-proliferative diabetic retinopathy (NPDR) with high-risk characteristics. This procedure involves applying numerous laser spots (typically 800-1600) to the peripheral retina, sparing the macula (the central part of the retina responsible for sharp, detailed vision). The aim is to destroy ischemic (oxygen-deprived) peripheral retinal tissue, which is believed to be the source of VEGF production. [3]
The Diabetic Retinopathy Study (DRS) and the Early Treatment Diabetic Retinopathy Study (ETDRS) established PRP as an effective treatment for reducing the risk of severe vision loss in PDR. While highly effective in preventing progression, PRP can lead to certain side effects, including decreased peripheral and night vision, and in some cases, mild reduction in central visual acuity. [4]
2. Focal and Grid Laser Photocoagulation
Focal and grid laser photocoagulation are used to treat diabetic macular edema (DME), a common complication of DR characterized by fluid accumulation in the macula, leading to blurred central vision. Focal photocoagulation targets specific leaking microaneurysms, while grid photocoagulation involves applying a pattern of light laser burns to areas of diffuse macular edema. [5]
The ETDRS demonstrated the efficacy of focal/grid laser treatment in reducing the risk of moderate vision loss and improving visual acuity in eyes with clinically significant DME. However, with the advent of anti-VEGF injections, laser treatment for DME is often used as an adjunct or in cases where anti-VEGF therapy is not fully effective or contraindicated. [6]
Mechanism of Action
Laser photocoagulation utilizes thermal energy to achieve its therapeutic effects. The laser light is absorbed by the melanin in the retinal pigment epithelium (RPE) and choroid, generating heat. This heat causes coagulation and destruction of the targeted tissue. In PRP, the destruction of ischemic peripheral retina reduces the metabolic burden and suppresses the release of angiogenic factors. In focal/grid laser, the treatment seals leaking microaneurysms and enhances the RPE pump function, thereby resolving macular edema. [7]
Indications and Clinical Guidelines
The decision to initiate laser treatment is guided by comprehensive clinical guidelines, such as those from the American Academy of Ophthalmology and the National Institute for Health and Care Excellence (NICE). Key indications include:
Proliferative Diabetic Retinopathy (PDR): Presence of high-risk PDR, characterized by new vessels on or within one disc diameter of the optic disc (NVD), new vessels elsewhere (NVE) with vitreous hemorrhage, or extensive NVE. [8]
Severe Non-Proliferative Diabetic Retinopathy (NPDR): In some cases, very severe NPDR may warrant PRP to prevent progression to PDR, especially if follow-up is uncertain. [9]
Diabetic Macular Edema (DME): Clinically significant DME, particularly if it is not responsive to anti-VEGF therapy or if anti-VEGF is not feasible. [10]
Efficacy and Outcomes
Laser photocoagulation has a long-standing history of proven efficacy in managing DR. Studies have consistently shown that PRP significantly reduces the risk of severe vision loss and blindness in patients with PDR. For DME, focal/grid laser has been effective in stabilizing and, in some cases, improving visual acuity. [11]
However, it is crucial to understand that laser treatment primarily aims to prevent further vision loss rather than to restore lost vision. It is a destructive procedure, and while beneficial, it can have side effects. The integration of anti-VEGF therapy has further refined the treatment paradigm for DR and DME, often making anti-VEGF the first-line treatment for DME, with laser used as a complementary or secondary option. [12]
✅ Tip: Early Detection is Key
Regular comprehensive eye exams are paramount for individuals with diabetes. Early detection of diabetic retinopathy allows for timely intervention, which can significantly improve visual outcomes and prevent severe vision loss.
ℹ️ Important Consideration: Combined Therapy
In many contemporary treatment protocols, laser photocoagulation is used in conjunction with other therapies, such as anti-VEGF injections, to achieve optimal outcomes in managing complex cases of diabetic retinopathy and macular edema.
نتیجہ اخذ کرنا
Laser treatment, particularly panretinal photocoagulation and focal/grid laser, remains a cornerstone in the management of diabetic retinopathy. While newer therapies like anti-VEGF injections have emerged, laser therapy continues to play a vital role, either as a primary treatment for PDR or as an adjunctive therapy for DME. Understanding its mechanisms, indications, and potential outcomes is essential for both clinicians and patients in navigating the complexities of diabetic eye disease and preserving precious vision.
✅ Key Takeaway
Laser photocoagulation is a critical and effective treatment for diabetic retinopathy, working to prevent severe vision loss by targeting abnormal blood vessels and reducing macular edema. Its role, often in combination with other therapies, underscores the importance of early detection and tailored management strategies for diabetic eye disease.
References
[1] National Eye Institute. (n.d.). Diabetic Retinopathy. Retrieved from https://www.nei.nih.gov/eye-health-information/eye-conditions-and-diseases/diabetic-retinopathy
[2] Healthline. (2023, July 6). Laser Treatment for Diabetic Retinopathy: What You Should Know. Retrieved from https://www.healthline.com/health/diabetes/laser-treatment-for-diabetic-retinopathy
[3] National Eye Institute. (n.d.). Laser Treatment for Diabetic Retinopathy. Retrieved from https://www.nei.nih.gov/eye-health-information/eye-conditions-and-diseases/diabetic-retinopathy/laser-treatment-diabetic-retinopathy
[4] Nature. (2025, December 4). NICE guidelines reaffirm the key role of laser for treating proliferative diabetic retinopathy. Retrieved from https://www.nature.com/articles/s41433-025-04129-x
[5] Kaiser Permanente. (n.d.). Laser Photocoagulation for Diabetic Retinopathy. Retrieved from https://healthy.kaiserpermanente.org/health-wellness/health-encyclopedia/he.laser-photocoagulation-for-diabetic-retinopathy.tf4075
[6] Retina Today. (n.d.). Laser Therapy for Diabetic Retinopathy and Diabetic Macular Edema. Retrieved from https://retinatoday.com/articles/2017-may-june/laser-therapy-for-diabetic-retinopathy-and-diabetic-macular-edema
[7] NIH. (n.d.). Laser management of diabetic retinopathy. Retrieved from https://pmc.ncbi.nlm.nih.gov/articles/PMC539507/
[8] Nature. (2025, December 4). NICE guidelines reaffirm the key role of laser for treating proliferative diabetic retinopathy. Retrieved from https://www.nature.com/articles/s41433-025-04129-x
[9] Eye Consultants of PA. (n.d.). What is Nonproliferative Diabetic Retinopathy Laser Treatment?. Retrieved from https://eyeconsultantsofpa.com/what-is-nonproliferative-diabetic-retinopathy-laser-treatment/
[10] ASRS. (2019, April 30). Evidence-Based Guidelines for Management of Diabetic Macular Edema. Retrieved from https://www.asrs.org/content/documents/evidence-based-guidelines-for-management-of-diabetic-macular-edema.pdf
[11] National Eye Institute. (n.d.). Laser Treatment Effective for Diabetic Retinopathy. Retrieved from https://www.nei.nih.gov/research-and-training/research-news/laser-treatment-effective-diabetic-retinopathy
[12] Diabetes Journals. (2023, December 11). 12. Retinopathy, Neuropathy, and Foot Care: Standards of Care in Diabetes—2024. Retrieved from https://diabetesjournals.org/care/article/47/Supplement_1/S231/153941/12-Retinopathy-Neuropathy-and-Foot-Care-Standards