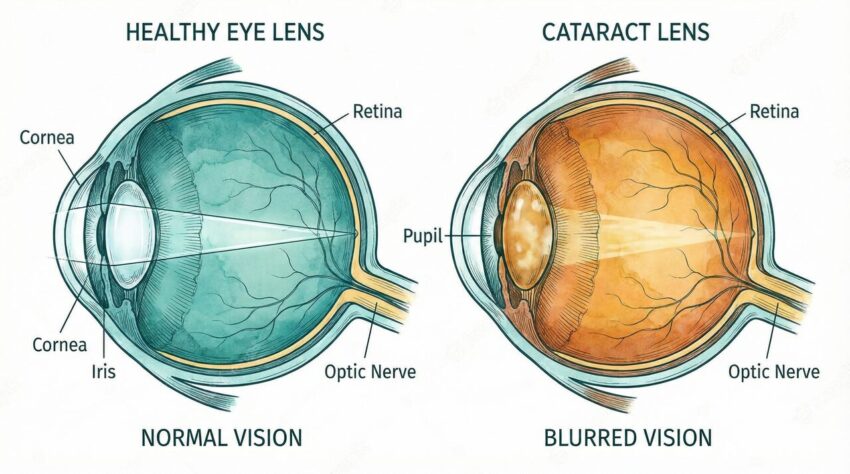
For many, the world slowly loses its sharpness, a gradual, painless blurring of vision that often signals the onset of cataracts. This clouding of the eye’s natural lens is a leading cause of vision loss globally, a seemingly inevitable part of aging. However, for millions living with diabetes, this process can be alarmingly accelerated, casting a shadow over their sight much earlier in life. Understanding the intricate connection between diabetes and cataracts is the first step toward protecting your vision. This article explores the science behind why people with diabetes are more susceptible to cataracts, what to look for, and the modern approaches to treatment that are helping people see clearly again.
The Science Behind Diabetic Cataracts
At its core, the link between diabetes and cataracts is a story of sugar. Chronic high blood sugar, or hyperglycemia, sets off a cascade of chemical reactions within the delicate environment of the eye’s lens, leading to the loss of its crystal-clear transparency. Three primary mechanisms are at play:
The Polyol Pathway: A Sugar Trap
When blood sugar levels are high, the lens takes in more glucose than it can handle. The excess glucose is shunted into an alternative metabolic route called the polyol pathway. Here, an enzyme named aldose reductase converts glucose into sorbitol, a sugar alcohol. Unlike glucose, sorbitol cannot easily exit the lens cells. As sorbitol accumulates, it creates an osmotic imbalance, pulling water into the lens and causing it to swell. This process disrupts the precise architecture of the lens fibers, contributing to their opacification. To make matters worse, this pathway consumes a vital molecule called NADPH, which is essential for regenerating the lens’s primary antioxidant, glutathione. The depletion of these antioxidant defenses leaves the lens vulnerable to oxidative damage.
Advanced Glycation End-Products (AGEs): The Browning Effect
High blood sugar also promotes a process called non-enzymatic glycation, where sugar molecules randomly attach to proteins in the lens, particularly the crystallins that are responsible for its transparency. Over time, these attachments lead to the formation of advanced glycation end-products, or AGEs. AGEs act like molecular glue, cross-linking the crystallin proteins, causing them to clump together, stiffen, and turn yellowish-brown. This is similar to the browning reaction that occurs when you toast a marshmallow. As AGEs accumulate, they progressively cloud the lens. They also generate harmful free radicals, adding to the oxidative stress within the eye.
ℹ️ The Power of Early Detection
Regular, comprehensive eye exams are crucial for everyone with diabetes. Early detection of cataracts and other eye conditions like diabetic retinopathy allows for timely intervention and can significantly improve long-term visual outcomes.
Oxidative Stress: The Final Blow
The polyol pathway and AGE formation work in tandem to create a perfect storm of oxidative stress. The lens is bombarded with reactive oxygen species (ROS), or free radicals, that outstrip its natural antioxidant defenses. This relentless oxidative assault damages the lens proteins and lipids, causing them to denature and aggregate. It is this cumulative damage that ultimately leads to the formation of a cataract, stealing away the clarity of vision.
Types of Cataracts in People with Diabetes
While diabetes can speed up the development of the same age-related cataracts that affect the general population, it is also linked to specific types of cataracts:
Accelerated Age-Related Cataracts: The most common scenario is the early onset and faster progression of nuclear sclerotic cataracts (a hardening and yellowing of the lens’s central core) and cortical cataracts (wedge-like opacities that form in the outer layers of the lens).
“True” Diabetic or “Snowflake” Cataracts: Though less common, these are a hallmark of poorly controlled diabetes, especially in younger individuals. They appear as a sudden burst of white, snowflake-like opacities just beneath the lens capsule and can progress very rapidly.
Posterior Subcapsular Cataracts (PSCs): These cataracts form on the back surface of the lens. They are particularly troublesome because their central location can cause significant glare and difficulty with reading, even in their early stages.
Recognizing the Signs: Symptoms and Diagnosis
The symptoms of diabetic cataracts are largely the same as other types of cataracts, but they often appear at a younger age and worsen more quickly. Be on the lookout for:
A gradual, painless blurring or dimming of vision.
Seeing halos or starbursts around lights, especially at night.
Increased sensitivity to glare from sunlight or headlights.
Difficulty seeing in low-light conditions.
Colors appearing faded or yellowish.
Frequent changes in your eyeglass or contact lens prescription.
If you have diabetes and experience any of these symptoms, it’s crucial to see an ophthalmologist. A comprehensive eye exam, including a slit-lamp examination to get a magnified view of your lens, is the only way to diagnose a cataract. Regular, dilated eye exams are essential for everyone with diabetes to catch cataracts and other eye problems, like diabetic retinopathy, as early as possible.
✅ Your Best Defense: Glycemic Control
Maintaining tight control over your blood sugar levels is the single most important thing you can do to prevent or slow the progression of cataracts. By keeping your blood glucose and HbA1c levels within your target range, you can minimize the harmful biochemical processes that damage the lens.
Taking Control: Management and Treatment
The best defense against diabetic cataracts is proactive management of your diabetes.
The Power of Glycemic Control
Maintaining tight control over your blood sugar levels is the single most important thing you can do to prevent or slow the progression of cataracts. By keeping your blood glucose and HbA1c levels within your target range, you can minimize the harmful biochemical processes that damage the lens.
Lifestyle Choices Matter
A healthy lifestyle provides an extra layer of protection. A diet rich in antioxidants from fruits and vegetables, regular exercise, and quitting smoking can all contribute to better eye health. Always wear sunglasses that block 100% of UV rays when you’re outdoors.
When Surgery is the Answer
When a cataract progresses to the point where it interferes with your daily activities—like reading, driving, or recognizing faces—surgery is the only effective treatment. Cataract surgery is one of the most common and successful surgical procedures performed today. It involves removing the clouded natural lens and replacing it with a clear, artificial intraocular lens (IOL).
For people with diabetes, the surgery requires some extra precautions. Your ophthalmologist will carefully evaluate the health of your retina to check for diabetic retinopathy. If significant retinopathy is present, it may need to be treated with laser therapy or injections before cataract surgery to ensure the best possible visual outcome. After surgery, it’s vital to continue managing your blood sugar diligently and follow your doctor’s instructions for using eye drops to prevent infection and inflammation.
Navigating Post-Surgery Complications
While cataract surgery is very safe, people with diabetes have a slightly higher risk of certain complications:
Posterior Capsule Opacification (PCO): Sometimes called a “secondary cataract,” this is a clouding of the membrane behind the new lens. It’s easily treated with a quick, painless laser procedure.
Cystoid Macular Edema (CME): This is swelling in the central part of the retina. It can be treated with anti-inflammatory eye drops or other medications.
Progression of Diabetic Retinopathy: In some cases, the inflammation from surgery can worsen existing diabetic retinopathy. Close monitoring after surgery is key.
Despite these risks, the vast majority of people with diabetes who undergo cataract surgery experience a dramatic improvement in their vision and quality of life. The key is a partnership between you, your endocrinologist, and your ophthalmologist to ensure your diabetes is well-managed before, during, and after the procedure.
✅ Key Takeaway
Cataracts are a serious complication of diabetes, but they are not an inevitability. Through diligent blood sugar control, a healthy lifestyle, and regular eye exams, you can significantly reduce your risk and protect your precious sense of sight. And if cataracts do develop, modern surgery offers a safe and effective path to restoring clear vision. By taking a proactive role in your eye health, you can look forward to a brighter, clearer future.