Introduction
In the intricate landscape of human health, certain conditions often intertwine, creating complex challenges that extend beyond their individual diagnoses. Diabetes, a pervasive metabolic disorder affecting millions globally, is one such condition. While much attention is rightly given to blood sugar management and its immediate complications, a less frequently discussed yet equally significant connection exists: the relationship between low testosterone, also known as hypogonadism, and diabetes, particularly Type 2. This article aims to demystify this crucial link, exploring how these two conditions influence each other and, more importantly, how understanding this connection can empower individuals to better manage their health.
Main Body
Understanding Low Testosterone (Hypogonadism)
Testosterone, often dubbed the primary male sex hormone, plays a far more expansive role than just reproductive health. It is a vital androgen produced primarily in the testes, influencing numerous bodily functions. Beyond its well-known effects on libido, sperm production, and the development of male secondary sexual characteristics, testosterone is crucial for maintaining bone density, muscle mass, red blood cell production, and even mood and cognitive function. It also plays a significant role in metabolic processes, including insulin sensitivity and fat distribution.
Hypogonadism refers to a condition where the body produces insufficient testosterone. This deficiency can manifest through a variety of symptoms that often overlap with other health issues, making diagnosis challenging. Common indicators include persistent fatigue, a noticeable decrease in libido, erectile dysfunction, and changes in mood such as irritability or depression. Physically, individuals might experience reduced muscle mass, an increase in body fat (particularly around the abdomen), and thinning bones (osteoporosis). Recognizing these symptoms is the first step toward understanding a potential underlying hormonal imbalance.
The Bidirectional Link: Diabetes and Low Testosterone
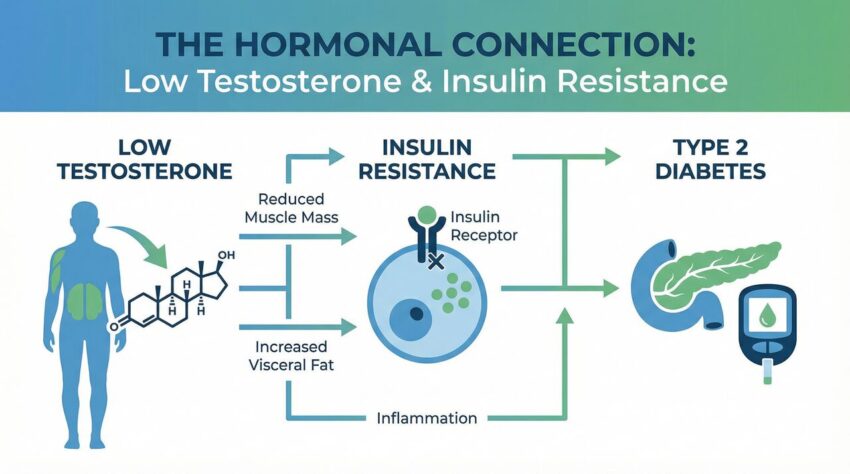
The relationship between diabetes and low testosterone is not merely coincidental; it is a complex, bidirectional interplay where each condition can exacerbate the other. This creates a challenging cycle that requires careful attention.
How Diabetes Contributes to Low Testosterone
Type 2 diabetes, characterized by insulin resistance and often accompanied by obesity, significantly increases the risk of developing low testosterone. Several mechanisms contribute to this:
- Insulin Resistance and Obesity: Excess adipose tissue, particularly visceral fat, is metabolically active and produces inflammatory cytokines and enzymes like aromatase, which converts testosterone into estrogen. This process directly lowers circulating testosterone levels. Insulin resistance itself can also impair testicular function and disrupt the delicate hormonal balance.
- Inflammation and Oxidative Stress: Chronic low-grade inflammation, common in individuals with diabetes, can damage the Leydig cells in the testes responsible for testosterone production. Similarly, increased oxidative stress can impair the function of these cells, leading to reduced testosterone synthesis.
- Impact on the Hypothalamic-Pituitary-Gonadal (HPG) Axis: The HPG axis is a complex feedback loop involving the hypothalamus, pituitary gland, and gonads that regulates testosterone production. Diabetes can disrupt this axis, leading to impaired signaling and consequently, lower testosterone levels. This often manifests as hypogonadotropic hypogonadism, where the brain signals for testosterone production are insufficient.
How Low Testosterone Impacts Diabetes Management
Conversely, low testosterone can worsen glycemic control and complicate diabetes management:
- Worsened Insulin Sensitivity: Testosterone plays a role in maintaining insulin sensitivity. Lower levels of the hormone are associated with increased insulin resistance, making it harder for the body to utilize glucose effectively and contributing to higher blood sugar levels.
- Increased Visceral Fat: Low testosterone can lead to an increase in visceral fat, the metabolically harmful fat stored around abdominal organs. This further fuels insulin resistance and inflammation, perpetuating the cycle.
- Negative Effects on Glucose Metabolism: Testosterone influences glucose uptake and metabolism in various tissues. Its deficiency can impair these processes, contributing to hyperglycemia.
- Potential for Increased Risk of Cardiovascular Disease: Both diabetes and low testosterone are independent risk factors for cardiovascular disease. Their coexistence can amplify this risk, highlighting the importance of addressing both conditions comprehensively.
Diagnosis and Screening
Given the strong association, screening for low testosterone is crucial for men with Type 2 diabetes. The diagnostic process typically involves a thorough assessment of symptoms, followed by blood tests. These tests measure total testosterone and, often, free testosterone levels, usually in the morning when levels are highest. Multiple measurements may be required to confirm a diagnosis, as testosterone levels can fluctuate. It is imperative to consult a healthcare provider if symptoms suggestive of low testosterone are present, especially for those already managing diabetes.
Management Strategies
Addressing low testosterone in the context of diabetes requires a multifaceted approach, often combining lifestyle modifications with medical interventions.
Lifestyle Interventions
These are foundational and can significantly impact both conditions:
- Weight Management: Losing excess weight, particularly visceral fat, is one of the most effective strategies. A balanced diet rich in whole foods and regular physical activity can improve insulin sensitivity and may naturally boost testosterone levels.
- Stress Reduction: Chronic stress elevates cortisol, which can negatively impact testosterone production. Techniques like mindfulness, meditation, and adequate relaxation are beneficial.
- Adequate Sleep: Sleep deprivation disrupts hormonal balance, including testosterone. Aim for 7-9 hours of quality sleep per night.
Testosterone Replacement Therapy (TRT)
When lifestyle changes are insufficient, Testosterone Replacement Therapy (TRT) may be considered. TRT involves administering exogenous testosterone to bring levels back into a healthy range. It is typically considered for men with clinically low testosterone levels and bothersome symptoms.
- Benefits: Studies have shown that TRT can lead to significant improvements in men with diabetes and hypogonadism. These benefits include improved glycemic control, reduced insulin resistance, increased muscle mass, decreased fat mass, and improvements in mood, energy levels, and libido. Some research even suggests TRT can contribute to the remission of Type 2 diabetes in a subset of patients.
“Testosterone replacement therapy has been shown to improve insulin sensitivity and glycemic control in hypogonadal men with type 2 diabetes, offering a promising avenue for comprehensive management.” – Journal of Clinical Endocrinology & Metabolism
- Risks and Considerations: TRT is not without potential risks and requires careful monitoring by a healthcare professional. Concerns include potential effects on prostate health (though studies have largely alleviated fears of causing prostate cancer, it can accelerate growth of existing cancers), cardiovascular effects, and polycythemia (an increase in red blood cells). Regular blood tests are essential to monitor testosterone levels, prostate-specific antigen (PSA), and red blood cell count.
Other Medications
In some cases, other medications might be used. For instance, metformin, a common diabetes medication, has shown some potential in improving testosterone levels in certain male patients, though its primary role remains glucose management.
Empathetic Approach and Patient Empowerment
Living with diabetes and potentially low testosterone can be challenging, but it is crucial to remember that these are common and manageable conditions. An empathetic approach from healthcare providers, coupled with proactive patient engagement, is key. Open communication with your doctor about all symptoms, concerns, and treatment preferences is vital. Focusing on holistic health—integrating diet, exercise, stress management, and appropriate medical care—empowers individuals to navigate these interconnected health challenges effectively.
Key Takeaways
- Low testosterone (hypogonadism) is significantly more prevalent in men with Type 2 diabetes.
- Diabetes and low testosterone share a bidirectional relationship, each worsening the other through mechanisms involving insulin resistance, obesity, and inflammation.
- Symptoms of low testosterone, such as fatigue, decreased libido, and changes in body composition, warrant discussion with a healthcare provider, especially for men with diabetes.
- Management involves lifestyle changes (weight loss, exercise, stress reduction, sleep) and, in some cases, Testosterone Replacement Therapy (TRT).
- TRT can improve glycemic control, insulin sensitivity, and overall well-being in hypogonadal men with diabetes, but requires careful medical supervision.
نتیجہ اخذ کرنا
The connection between low testosterone and diabetes is a critical area of health that deserves greater awareness. By understanding how these conditions interact, individuals can work more effectively with their healthcare teams to identify, diagnose, and manage both. Proactive screening, comprehensive lifestyle adjustments, and appropriate medical interventions, including TRT when indicated, offer pathways to improved metabolic health and an enhanced quality of life. Remember, managing diabetes is a journey, and addressing all contributing factors, including hormonal balance, is a powerful step towards overall well-being. Always consult your healthcare provider for personalized advice and treatment plans.