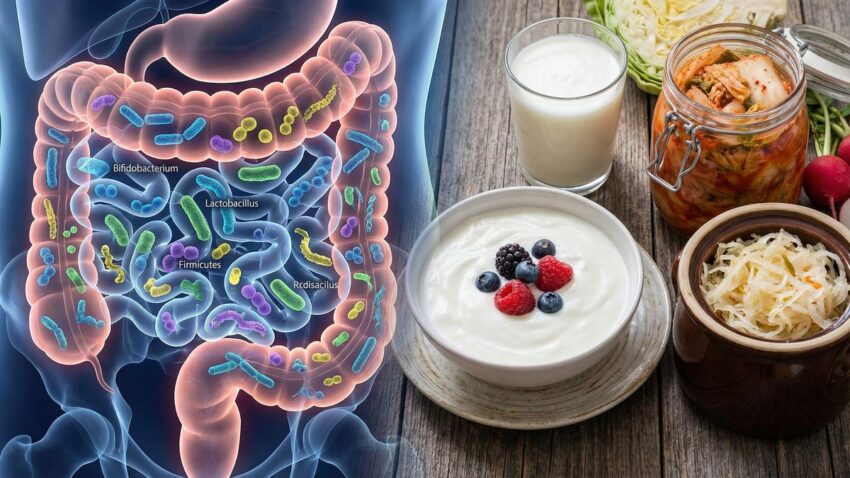
Recent research has revealed a fascinating connection between the trillions of microorganisms living in our digestive system and type 2 diabetes. This invisible ecosystem—our gut microbiome—may hold keys to understanding why diabetes develops and how we might prevent or manage it more effectively. This article explores the growing evidence linking gut health to blood sugar control and what it means for people living with diabetes.
Understanding the Gut Microbiome: Your Internal Ecosystem
Imagine a bustling city of trillions of microscopic residents living inside your digestive tract. This is your gut microbiome—a complex community of bacteria, viruses, fungi, and other microorganisms that have evolved alongside humans for millennia. Far from being passive hitchhikers, these tiny inhabitants play crucial roles in digestion, immunity, and even how our bodies process nutrients.
The average human gut contains approximately 100 trillion microorganisms representing over 1,000 different species. Together, they weigh about 2-5 pounds—roughly the weight of your brain! This vast community contains more genes than our human genome, earning it the nickname “the forgotten organ.”
ℹ️ Did You Know?
Your gut microbiome contains approximately 100 trillion microorganisms—about 10 times more microbial cells than human cells in your entire body! These microbes collectively contain over 3 million genes, compared to the approximately 23,000 genes in the human genome.
What makes a healthy microbiome? Diversity is key. Research consistently shows that people with a wide variety of beneficial microbes tend to have better health outcomes than those with less diverse gut communities. This diversity acts like an ecological safety net, making the entire system more resilient and functional.
The Gut-Diabetes Connection: What Science Reveals
Over the past decade, researchers have uncovered compelling evidence linking gut microbiome imbalances (dysbiosis) to type 2 diabetes. Several landmark studies have shown that people with type 2 diabetes often have distinctly different gut microbiome compositions compared to those without the condition.
A 2020 review published in the journal Cell Host & Microbe analyzed data from multiple studies and found consistent patterns: people with type 2 diabetes typically show reduced microbial diversity, fewer beneficial bacteria that produce short-chain fatty acids, and more potentially harmful inflammatory bacteria.
But how exactly does the microbiome influence diabetes? Scientists have identified several mechanisms:
Insulin Resistance and Inflammation
Certain gut bacteria produce compounds that can trigger chronic, low-grade inflammation—a key factor in insulin resistance. When the gut lining becomes more permeable (sometimes called “leaky gut”), bacterial components can enter the bloodstream, prompting immune responses that interfere with insulin signaling.
Research published in Nature found that lipopolysaccharides (LPS)—components from the outer membrane of certain bacteria—can trigger inflammatory responses that impair insulin sensitivity. Higher levels of these bacterial endotoxins have been observed in people with type 2 diabetes.
Short-Chain Fatty Acids: The Metabolic Messengers
When beneficial gut bacteria ferment dietary fiber, they produce compounds called short-chain fatty acids (SCFAs)—primarily acetate, propionate, and butyrate. These SCFAs serve as important messengers between the gut and other body systems.
Studies show that SCFAs help regulate blood glucose levels by:
- Improving insulin secretion from pancreatic beta cells
- Enhancing insulin sensitivity in muscle and liver tissues
- Reducing inflammation throughout the body
- Influencing appetite regulation and metabolism
People with type 2 diabetes often have fewer SCFA-producing bacteria, potentially contributing to their metabolic challenges.
Bile Acid Metabolism
Gut bacteria help transform bile acids (produced by the liver to aid digestion) into secondary bile acids. These modified bile acids act as signaling molecules that influence glucose metabolism and energy expenditure.
Research suggests that altered bile acid metabolism due to microbiome changes may contribute to metabolic disorders, including type 2 diabetes.
| Microbiome Characteristics | Typical in Healthy Metabolism | Typical in Type 2 Diabetes |
|---|---|---|
| Microbial Diversity | High diversity | Reduced diversity |
| SCFA-Producing Bacteria | Abundant | Decreased |
| Inflammatory Bacteria | Lower levels | Higher levels |
| Gut Barrier Function | Strong integrity | Often compromised |
Nurturing Your Gut for Better Blood Sugar Control
The exciting news is that your gut microbiome isn’t fixed—it’s highly responsive to lifestyle factors, particularly diet. Here are evidence-based strategies for cultivating a diabetes-friendly gut ecosystem:
Embrace Dietary Fiber: Fuel for Beneficial Bacteria
Fiber-rich foods act as prebiotics—substances that feed beneficial gut bacteria. When these bacteria ferment fiber, they produce those valuable SCFAs that improve metabolic health.
Research published in Science found that people consuming high-fiber diets had greater microbial diversity and improved glucose metabolism. Aim for a variety of fiber sources, including:
- Vegetables: broccoli, Brussels sprouts, artichokes
- Fruits: berries, apples, pears (with skin)
- Legumes: beans, lentils, chickpeas
- Whole grains: oats, barley, quinoa
- Nuts and seeds: flaxseeds, chia seeds, almonds
✅ Practical Tip
When increasing fiber intake, do so gradually over several weeks to minimize digestive discomfort. Aim for at least 25-30 grams daily, and pair increased fiber with plenty of water. If you have concerns about how specific high-fiber foods might affect your blood sugar, use your glucose monitor to observe your body’s unique response.
Consider Fermented Foods: Living Microbial Allies
Fermented foods contain live beneficial bacteria (probiotics) that can temporarily colonize your gut and influence your resident microbiome. Research from Stanford University found that a diet rich in fermented foods increased microbiome diversity and reduced inflammatory markers.
Diabetes-friendly fermented options include:
- Unsweetened yogurt with live cultures
- Kefir (fermented milk drink)
- Sauerkraut and kimchi
- Tempeh
- Kombucha (check sugar content)
Limit Ultra-Processed Foods and Artificial Sweeteners
Highly processed foods and some artificial sweeteners appear to disrupt the gut microbiome. A 2021 study in Cell found that certain emulsifiers and preservatives common in processed foods altered gut bacteria in ways that promoted inflammation and metabolic dysfunction.
Similarly, research suggests some artificial sweeteners may alter gut bacteria composition in ways that paradoxically impair glucose tolerance—the opposite of their intended effect.
Consider the Mediterranean Diet Pattern
The Mediterranean diet—rich in vegetables, fruits, olive oil, nuts, fish, and whole grains—has been shown to promote a healthy gut microbiome while also improving glycemic control. A landmark study in the British Medical Journal found that this eating pattern increased beneficial bacteria while reducing diabetes risk by up to 30%.
Beyond Diet: Other Factors That Shape Your Gut Microbiome
While diet has the strongest influence on gut health, other lifestyle factors also matter:
Physical Activity
Regular exercise appears to enhance microbiome diversity and increase beneficial bacteria. Research in Medicine & Science in Sports & Exercise found that athletes had greater microbial diversity than sedentary individuals, with higher levels of bacteria that produce beneficial SCFAs.
Stress Management
The gut-brain connection is bidirectional—stress affects gut function, and gut health influences stress responses. Chronic stress can alter gut bacteria composition in ways that promote inflammation and metabolic problems. Practices like meditation, adequate sleep, and social connection support both mental wellbeing and gut health.
Medication Considerations
Some medications, particularly antibiotics, can dramatically alter the gut microbiome. While antibiotics are sometimes necessary, using them judiciously helps preserve microbiome integrity. Interestingly, the diabetes medication metformin appears to have beneficial effects on the gut microbiome, which may contribute to its therapeutic benefits.
ℹ️ Did You Know?
Research suggests that metformin, the most commonly prescribed medication for type 2 diabetes, may work partly through its effects on gut bacteria. Studies show it increases beneficial Akkermansia bacteria, which are associated with better metabolic health and enhanced gut barrier function.
The Future: Microbiome-Based Therapies for Diabetes
The growing understanding of the gut-diabetes connection is opening exciting new therapeutic possibilities:
Personalized Nutrition
Emerging research suggests that people have individualized blood sugar responses to the same foods, partly due to differences in their gut microbiomes. Future diabetes management may include personalized dietary recommendations based on microbiome analysis.
Targeted Probiotics
Scientists are working to develop next-generation probiotics specifically designed to improve glucose metabolism. Unlike general probiotics, these would contain specific bacterial strains proven to influence pathways involved in diabetes.
Fecal Microbiota Transplantation
Early clinical trials are exploring fecal microbiota transplantation (FMT)—transferring gut bacteria from healthy donors to people with metabolic disorders. While still experimental, some studies show promising improvements in insulin sensitivity following FMT.
✅ Key Takeaway
The gut microbiome plays a significant role in type 2 diabetes development and management. While research is still evolving, there’s strong evidence that nurturing your gut health through a fiber-rich diet, fermented foods, regular physical activity, and stress management can positively impact blood sugar control. These microbiome-friendly habits align with established diabetes management recommendations, making them valuable additions to your health toolkit. As science advances, microbiome-based approaches may become increasingly important in personalized diabetes care.
Disclaimer: The information provided in this article is for educational purposes only and should not replace professional medical advice. Always consult with your healthcare team before making changes to your diabetes management plan.