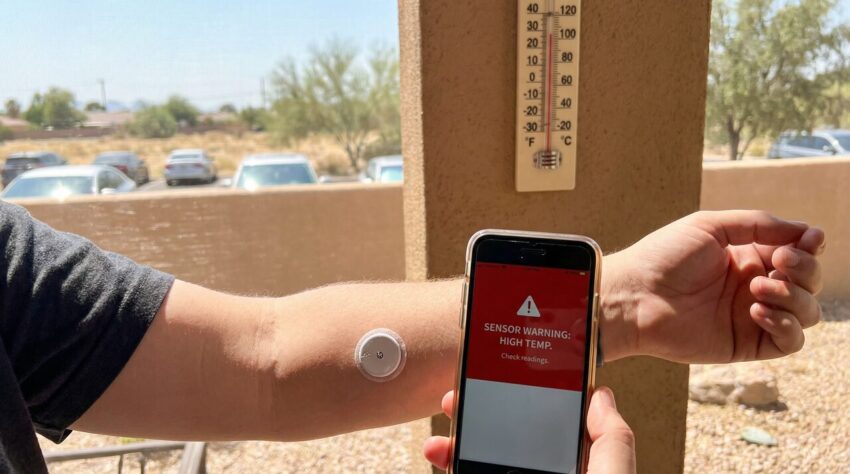
CGM Accuracy in Extreme Heat: Navigating Diabetes Management in Rising Temperatures
For many individuals managing diabetes, Continuous Glucose Monitors (CGMs) have become an indispensable ally, offering real-time insights into glucose fluctuations and empowering informed health decisions. However, the reliability of these sophisticated devices is not immune to environmental influences. Extreme heat, in particular, presents a notable challenge, potentially compromising CGM accuracy. As global temperatures continue to climb, a thorough understanding of how heat impacts CGM performance, coupled with proactive mitigation strategies, becomes paramount for sustaining effective diabetes management.
Understanding CGM Sensitivity to Heat
Continuous Glucose Monitors, while marvels of modern technology designed for precise glucose measurement, are nonetheless susceptible to external conditions. Elevated temperatures can disrupt the delicate internal mechanisms of the sensor, leading to potentially skewed or unreliable data. This inherent sensitivity is a crucial consideration for all CGM users, especially during periods of intense heat or in consistently warm climates.
How Heat Affects CGM Sensors
The ways in which extreme heat can undermine CGM accuracy are multifaceted. Primarily, the biochemical reactions occurring within the sensor, fundamental to glucose detection, can be significantly altered by high temperatures. This alteration may manifest as either spuriously elevated or diminished readings, thereby obscuring genuine glucose trends. Furthermore, the adhesive responsible for securing the sensor to the skin is prone to degradation under prolonged thermal stress, heightening the risk of premature detachment. A sensor that is loose or dislodged will invariably yield inaccurate data. Lastly, the electronic components, most notably the transmitter’s battery, are vulnerable to adverse effects from high temperatures, potentially resulting in device malfunction or a curtailed operational lifespan. Most CGM manufacturers stipulate specific operating temperature ranges, frequently cautioning against exposure to temperatures exceeding 37°C (98.6°F) or 40°C (104°F) [1, 2]. Transgressing these limits can substantially impair device performance.
Recognizing Inaccurate Readings
It is incumbent upon CGM users to cultivate an awareness of indicators suggesting potential inaccuracies in their device’s readings. Discrepancies between one’s physiological sensations and the glucose values displayed by the CGM, or sudden, inexplicable shifts in glucose levels, should serve as immediate alerts. While CGMs offer unparalleled convenience, they do not universally supersede traditional blood glucose meters (BGMs). In situations where CGM readings appear dubious, particularly amidst extreme heat, corroborating these values with a BGM is a judicious step to ensure accurate glucose monitoring. This practice not only validates CGM data but also instills confidence in one’s diabetes management.
Practical Strategies for Protecting Your CGM in Hot Weather
Implementing proactive measures can substantially diminish the adverse effects of extreme heat on both CGM functionality and user comfort. By embracing a few straightforward strategies, individuals can effectively safeguard their devices and uphold consistent glucose monitoring.
Keeping Your Sensor Cool
Shielding the sensor from direct thermal exposure is paramount. Wearing loose-fitting, breathable attire can establish a physical barrier against direct solar radiation and aid in regulating the skin temperature surrounding the sensor. Moreover, purpose-designed patch covers or armbands can furnish an additional stratum of protection and stability. It is imperative to refrain from leaving CGMs or their constituent parts in thermally oppressive environments, such as the interior of a parked vehicle, where temperatures can escalate rapidly. When venturing outdoors, consider utilizing an insulated bag equipped with a cooling gel pack for storing receivers or smartphones, ensuring that the cooling element does not come into direct contact with the device [2].
Managing Adhesive Challenges Due to Sweat
Elevated perspiration, a common consequence of hot weather, can compromise the efficacy of the sensor’s adhesive, thereby precipitating premature detachment. To counteract this, barrier wipes, such as Skin Tac or IV Prep, can be applied to the skin prior to sensor insertion, fostering a more robust and enduring bond. Furthermore, sweat-resistant overlay patches are available and can provide supplementary reinforcement. When undertaking sensor replacement, allowing the skin to thoroughly cool and dry before application can significantly enhance adhesion. Should the adhesive become moistened, gently patting it dry, rather than abrasive rubbing, can help preserve its integrity [2].
Water Activities and CGM Use
For individuals who partake in swimming or other aquatic pursuits, a clear understanding of their specific CGM model’s waterproof rating is indispensable. While most CGMs exhibit water resistance, not all are engineered for prolonged submersion. It is prudent to observe the manufacturer’s recommended
“settling” period (often 1–24 hours) subsequent to sensor insertion before engaging in water-based activities. The deployment of waterproof CGM covers or bands can confer an additional layer of safeguarding. Following aquatic exposure, rinsing the skin with clean water is beneficial for removing chlorine or saline residues, which possess the potential to irritate the integument or diminish adhesive longevity [2].
Protecting Companion Devices (Phones, Pumps)
Many contemporary CGM systems seamlessly integrate with smartphones or insulin pumps, rendering these ancillary devices equally critical for protection against extreme thermal conditions. Analogous to CGMs, both phones and pumps are susceptible to overheating, which can culminate in diminished functionality or irreversible damage. Maintaining these devices within shaded areas, or encasing them in insulated pouches augmented with cooling strips, can effectively avert thermal overload. Furthermore, it is judicious to deactivate superfluous background applications on smartphones to curtail endogenous heat generation. Direct contact between phones and heated skin, particularly when concealed beneath clothing or within armbands during physical exertion, should be assiduously avoided, as this can facilitate the transfer of body heat to the device [2].
The Body’s Response to Heat and Glucose Levels
Beyond the direct ramifications for medical devices, extreme heat exerts a profound influence on human physiology, which, in turn, modulates glucose regulation and consequently impacts CGM readings. A comprehensive grasp of these physiological adaptations is indispensable for holistic diabetes management during periods of elevated ambient temperatures.
Dehydration and Insulin Sensitivity
Elevated temperatures invariably augment the propensity for dehydration, a physiological state capable of elevating blood glucose concentrations. Dehydration effectively concentrates blood glucose, thereby yielding spuriously higher readings. Moreover, extreme heat can induce alterations in both the absorption kinetics and overall efficacy of insulin. Certain individuals may experience an augmented insulin sensitivity, predisposing them to a heightened risk of hypoglycemia, whilst others might observe a diminished efficiency of their insulin, potentially leading to hyperglycemia. The body’s intrinsic stress response to thermal extremes can also trigger the release of hormones that further elevate blood glucose levels, thereby orchestrating a complex interplay of factors necessitating meticulous monitoring [3].
Importance of Hydration
Maintaining adequate hydration stands as arguably one of the most pivotal strategies for navigating diabetes in hot climates. Water is instrumental in facilitating thermoregulation and plays a crucial role in glucose metabolism. Individuals with diabetes should endeavor to consume copious amounts of water throughout the day, irrespective of whether they perceive thirst. The avoidance of sugary beverages, which can further perturb blood glucose homeostasis, is equally significant. Electrolyte-rich fluids may confer additional benefits, particularly during protracted physical activity or episodes of profuse perspiration, but their selection should be undertaken with circumspection to preclude excessive sugar intake [3].
Key Takeaways
- Monitor CGM Readings Closely: Be vigilant for unusual patterns or discrepancies and cross-reference with a BGM if in doubt.
- Protect Devices from Direct Heat: Keep CGMs, phones, and pumps out of direct sunlight and hot environments.
- Reinforce Adhesion: Use barrier wipes and overlay patches to prevent sensor detachment due to sweat.
- Stay Hydrated: Drink plenty of water and avoid sugary beverages to help regulate blood glucose and body temperature.
- Consult Your Healthcare Provider: Discuss personalized strategies for managing diabetes and CGM use in hot weather.
Conclusion
The judicious management of diabetes amidst extreme thermal conditions presents a unique constellation of challenges. Nevertheless, armed with informed strategies and a proactive approach to care, individuals utilizing CGMs can successfully uphold accurate monitoring and achieve effective glycemic control. By internalizing the multifaceted ways in which heat influences both their medical devices and their physiological responses, and by diligently implementing practical protective measures, people living with diabetes can confidently embrace warmer weather. It is paramount to remember that your healthcare provider remains your most invaluable resource for bespoke advice and unwavering support. Remain composed, maintain optimal hydration, and persistently monitor your glucose levels with diligence to safeguard your overall well-being.
References
[1] Snaq.ai. “7 Factors That Affect Your CGM Accuracy.” Snaq.ai Blog, Accessed March 14, 2026. https://www.snaq.ai/blog/7-factors-that-affect-your-cgm-accuracy-sensor-placement-medications-and-more
[2] Love My Libre. “Beat the Heat: Tips to Protect your CGM during a Heatwave.” Love My Libre Blog, July 2, 2025. https://lovemylibre.com/blogs/news/tips-to-protect-sensor-cgm-during-heatwave
[3] CDC. “Managing Diabetes in the Heat.” Centers for Disease Control and Prevention, May 15, 2024. https://www.cdc.gov/diabetes/articles/managing-diabetes-in-the-heat.html